Vaccine to neutralise malaria
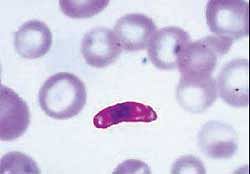
In early November, scientists at the Wellcome Trust Sanger Institute had found that Plasmodium falciparum — the deadliest strain of malaria parasite — relies on a single receptor, known as ‘basigin’, on the surface of red blood cells to invade the cell.
The parasite attaches a protein — the antigen RH5 — to the receptor, in a sense “unlocking” the doorway for the parasite to enter the red blood cell. Once there, it grows and replicates, causing potentially life-threatening disease.
Now, a team of scientists led by Dr Simon Draper from the Jenner Institute, at the University of Oxford, demonstrated that a vaccine they have developed induces an antibody response in animal models capable of neutralising all the tested strains of the P. falciparum parasite.
“Our initial finding, reported last month, was unexpected and completely changed the way in which we view how the malaria parasite invades red blood cells,” said Gavin Wright, of the Wellcome Trust Sanger Institute, who co-authored the study that published in the journal Nature Communications.
“It revealed what we think is the parasite’s Achilles’ heel in the way it invades our cells and provided a target for potential new vaccines.”
Dr Sandy Douglas, first author on the new study, added: “We have created a vaccine that confirms the recent discovery relating to the biology of RH5, given it can generate an immune response in animal models capable of neutralising many — and potentially all — strains of the P. falciparum parasite.
“It is an important step towards developing a much-needed vaccine against one of the world’s major killers.”
According to the researchers, the antigens of the malaria parasite are often genetically very diverse as they are forced to evolve to stay one step ahead of the immune system and avoid recognition by antibodies.
However, the RH5 antigen appears to have little genetic diversity. The researchers believe that this is because even people who have been naturally and repeatedly exposed to malaria have low or undetectable levels of antibodies that target this particular antigen.
These very low levels of antibody would be insufficient to kill the parasites, and hence would not exert a selective pressure for the antigen to evolve variability, they said.
Prof Adrian Hill, a Wellcome Trust senior investigator at the University of Oxford, said: “Vaccines against malaria are notoriously difficult to develop because the parasites’ antigens – the target of vaccines – tend to be genetically so diverse. The RH5 antigen doesn’t show this diversity, making it a particularly good target for a vaccine to exploit.
“Our next step will be to begin safety tests of this vaccine. If these prove successful, we could see clinical trials in patients beginning within the next two to three years.”
According to the World Malaria Report 2010, malaria killed an estimated 781,000 people in 2009, mainly young children and pregnant women.
Deccan Herald is on WhatsApp Channels| Join now for Breaking News & Editor's Picks